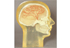
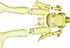
X-Ray & Radiography Phantoms
Supertech offers the most complete selection X-ray and Radiology Anthropomorphic Phantoms available.
Phantom selection includes: Full body, head, chest, abdomen, pelvis, arms, hands, legs, digital quality control, and feet. You may select from natural bone or synthetic bone, as well as opaque or transparent Phantoms.
Our knowledgeable staff can help you with your selection,
Supertech offers the most competitive pricing!
Phantom selection includes: Full body, head, chest, abdomen, pelvis, arms, hands, legs, digital quality control, and feet. You may select from natural bone or synthetic bone, as well as opaque or transparent Phantoms.
Our knowledgeable staff can help you with your selection,
Supertech offers the most competitive pricing!
Anthropomorphic Phantoms are hand made to order.
Manufacturing lead times can be as short as 4 weeks and as long as 14 weeks.
Plan your purchasing to allow time in manufacturing.
Please call for current lead times.